Meet our AI, Daniel
Your system for turning denied claims into collected revenue.
The reality is simple. Teams cannot keep up with the volume of denials.
So most of them sit untouched.
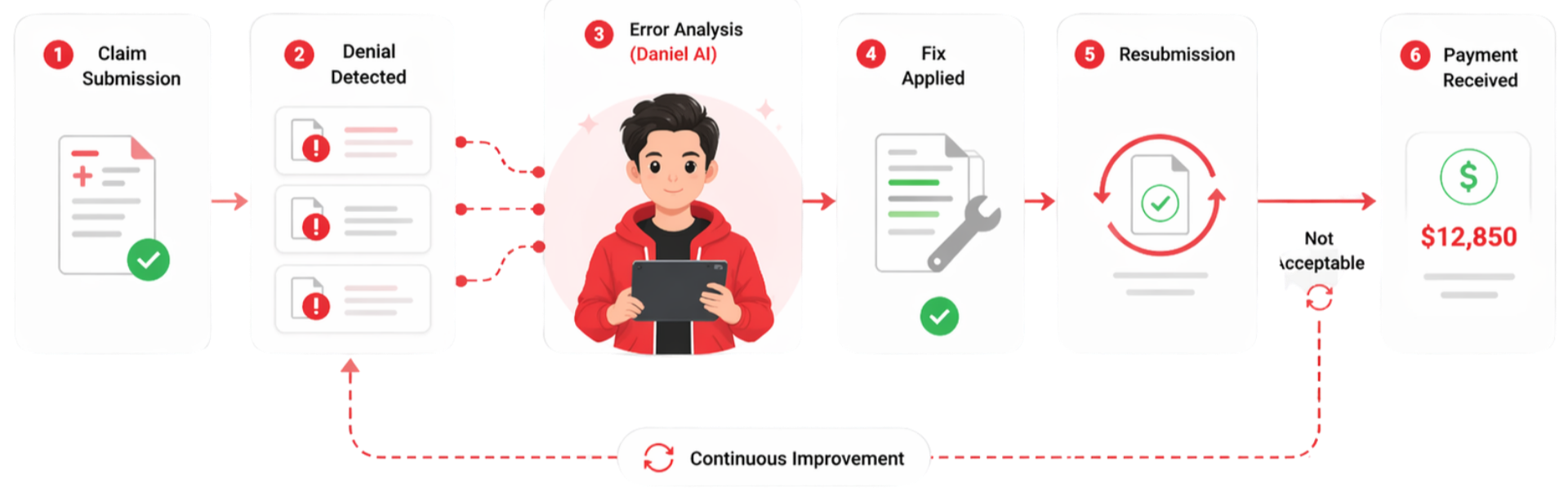
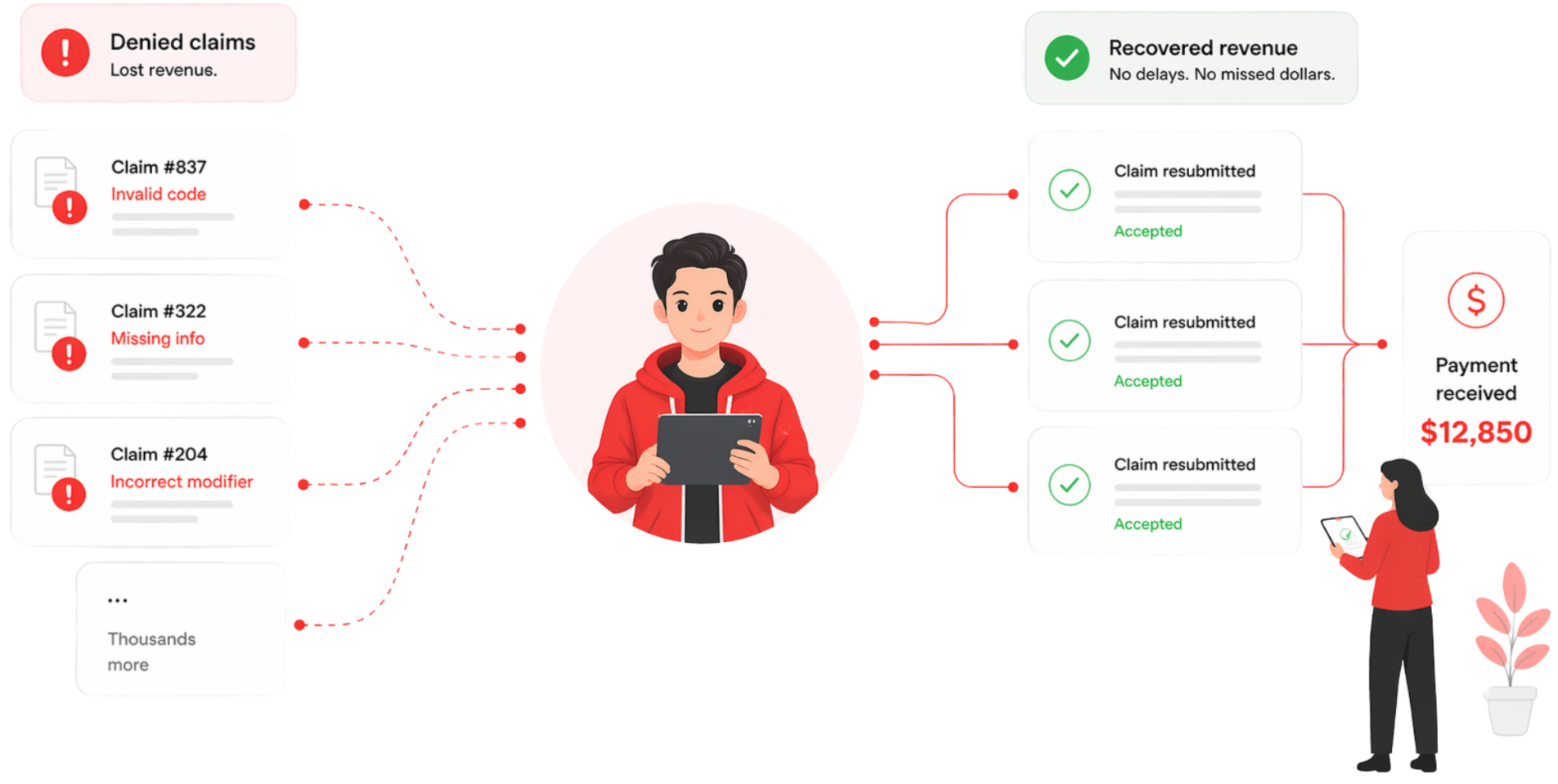
Daniel removes that limit.
It finds what went wrong. Applies the right fix. Sends the claim back out.
Powered by machine learning and healthcare trained GenAI, Daniel turns missed revenue into recovered revenue automatically.
Identify
We analyze denied claim lines across payers, policies, and coding patterns to surface high-confidence opportunities for recovery.
Remediate
Each denial is evaluated and corrected using structured, payer-specific logic to maximize the likelihood of approval.
Recover
Corrected claims are returned for payment at scale, ensuring every viable denial is processed without manual constraint.

Daniel The What
Daniel is our AI platform that uses advanced AI algorithms to automatically identify reasons for denials and how to solve them
Daniel uses large denial datasets for proprietary algorithms to automatically make corrections to denied claims
Daniel delivers automated claims submission to send corrected claims through the system to optimize revenue recovery
Daniel The How