Stop Writing Off Denials That Can Be Recovered Automatically
Our AI automatically identifies, fixes and resubmits health insurance claims denials at scale
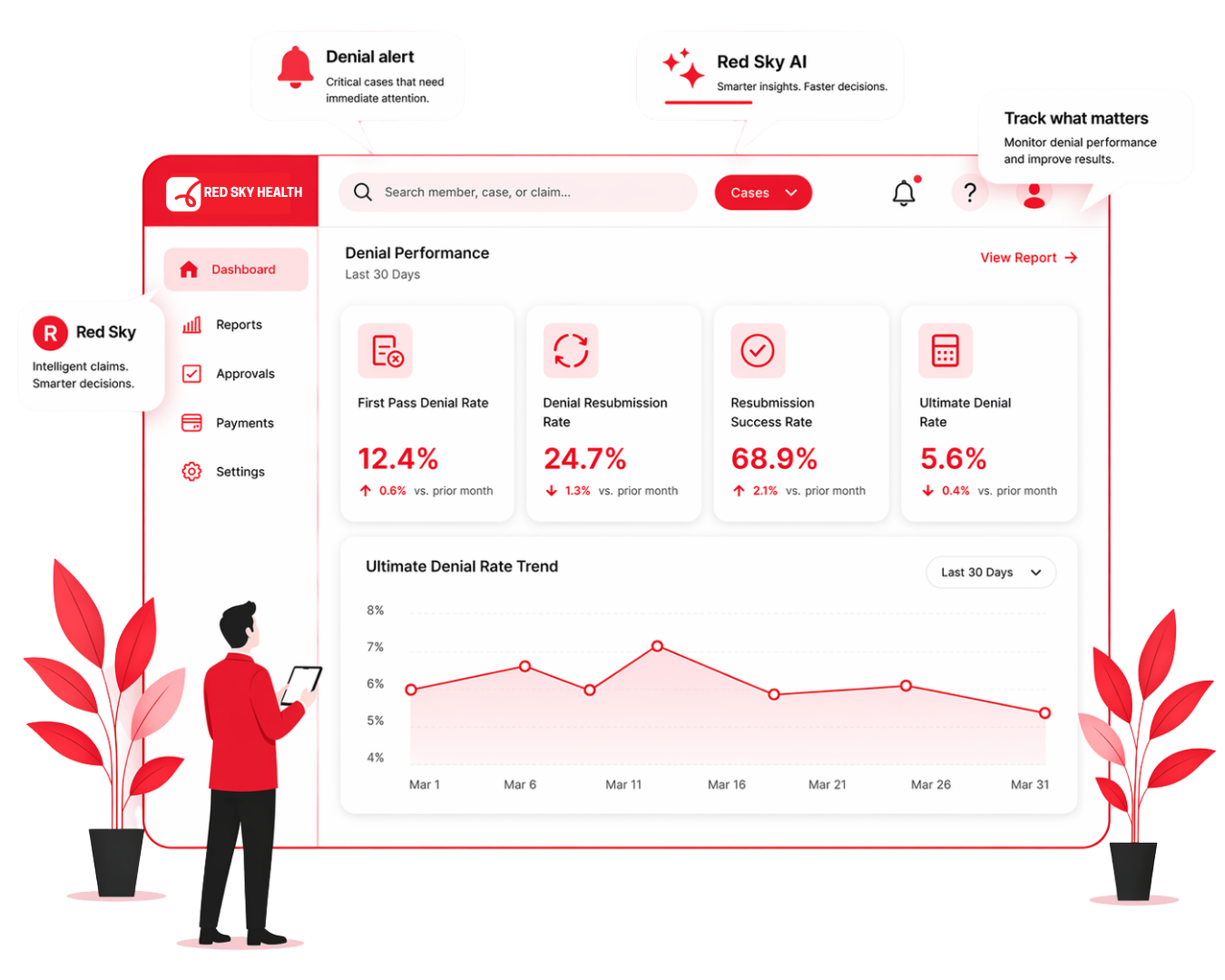
Most Denial Reporting Understates Real Loss
The challenge is not just the volume of denials. It is the lack of visibility into how denials are actually performing.
To understand the full picture of your denial performance, Red Sky Health offers a free Denials Analysis.

Your End-to-End Denials Remediation Platform
One end-to-end denials platform — built to identify, correct and resubmit denials at scale.
Comprehensive dashboard tracking denial charges, counts, and remitted amounts across all payers. Monitor sum of denial charges grouped by check issue date and denial reason with real-time updates.
Advanced AI analyzes each denial with complete claim context including coverage validity, benefit plan details, and authorization requirements. Surfaces critical information like ICD-10 codes, procedure codes, and payer-specific coverage limitations instantly.
Centralized state assignment and workflow management for all denials. Track each denial through states like "In Assignment", organize by payer, CPT codes, total billed and allowed amounts, with complete audit trails and team member assignments.
Intelligent claims management dashboard with queue filtering and automated resubmission workflows. View claim lists with facility, patient, payer, and status details. Streamline fixing and resubmission with one-click automation for faster revenue recovery.
Healthcare Providers - Are Insurance Claims Denials a Challenge?
Meet Daniel - Our AI Denials Remediation Platform

Daniel uses a large paid & denied claims dataset along with remittance information as the base for its AI models

Daniel uses this dataset for training its models and testing for better accuracy to remediate future denials
Daniel uses ML and LLMs to programmatically remediate and re-submit denials in real-time
Customer Testimonials
You May Already Be Writing Off Recoverable Revenue
Many losses hide inside partially paid claims, line-item denials, and write-offs no one sees clearly. We uncover and recover them.




